
This article was updated on January 12th, 2024

Making the decision to euthanize a dog with Cushing’s disease is not easy;. Due to the slow progression of the disease, we, as vets, often build strong bonds with the pets through the many years of treatment and management of the disease. This article specifically focuses on the final stages and the signs that your dog is dying from Cushing’s disease.
In our article on euthanizing a dog with Cushing’s disease, we reviewed the story of Millie, a 9-year-old Terrier, who I recently had to euthanize due to complications related to Cushing’s disease. With regular blood tests and changes to the drug we used, Millie manage to live a happy life for about two years.
However, one day, the owner had concerns that her behavior had changed, and she had started to become more aggressive at times. Unfortunately, her situation deteriorated quickly, with obvious neurological changes that impacted her behavior.
Let’s now review the signs and symptoms in the advanced stages of the disease.
Signs That Your Dog Is Dying from Cushing’s Disease
Signs that your dog is in the advanced stages of the disease include the following:
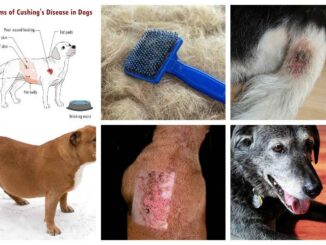
- Dogs will often develop a pot-bellied appearance, lose hair on their flanks and develop thin skin, as well as have recurrent infections due to an impaired immune system. While treatment aims to control these symptoms as best as possible, hyperadrenocorticism is a disease that gradually becomes harder to control as the tumor present in the pituitary or adrenal gland enlarges.

- A dog in the end stage of Cushing’s will be refractory to changes in medication; they are likely on the highest possible dose.
- Symptoms will often start to recur to the point where the dog is very lethargic, has an uncontrollable thirst and/or urination, and has repeated infections such as skin infections or urinary tract infections.
- Dogs with the pituitary-dependent form of hyperadrenocorticism can start to develop neurological abnormalities as an expanding pituitary gland tumor puts pressure on the surrounding brain tissue. If your dog is displaying symptoms such as nervousness, aggression, disorientation, circling, or even seizures, then a pituitary tumor is the likely cause. Unfortunately, not much can be done in this case if they are non-respondent to increased doses of medication.
Making the final decision to euthanize a dog with Cushing’s is not an easy one to make. Hyperadrenocorticism tends to be a slowly progressing disease in which symptoms gradually worsen over time. As such, there is usually not a clear-cut moment when a dog deteriorates.
Key questions to ask yourself
Your dog’s quality of life is the most important consideration when deciding when to euthanize. Ask yourself:
- Do they still seem interested in their favorite things, and are they still excited to greet you when you come home?
- Do they get out of breath easily, and are they reluctant to do any form of exercise?
- Do they get repeated infections?
- Are they constantly wanting to drink more water, and do they pee around the house?
- Do they show any neurological abnormalities?
If the answer to these questions is not a positive one, then it is the right time to consider euthanasia – talk to your vet, as they can help you come to the right conclusion. We also recommend you take our euthanasia quiz with 6 questions to answer to help you think through your dog’s quality of life.
Related Posts about Cushing’s Disease:
 Dog Cushing’s Disease Impact on Back Legs: Our Vet Explains - In my years as a veterinarian, I've frequently come across Cushing's disease in dogs, a… [...]
Dog Cushing’s Disease Impact on Back Legs: Our Vet Explains - In my years as a veterinarian, I've frequently come across Cushing's disease in dogs, a… [...] Cushing’s Disease Neurological Signs in Dogs - In my years as a veterinarian, I've frequently come across Cushing's disease in dogs, a… [...]
Cushing’s Disease Neurological Signs in Dogs - In my years as a veterinarian, I've frequently come across Cushing's disease in dogs, a… [...] Pictures of Cushing’s Disease in Dogs, with Vet Explanations - This article presents 10 pictures of Cushing's disease in dogs to illustrate its most common… [...]
Pictures of Cushing’s Disease in Dogs, with Vet Explanations - This article presents 10 pictures of Cushing's disease in dogs to illustrate its most common… [...] What is My Dog’s Life Expectancy With Cushing’s Disease? A Vet Weighs In - Essentially, Cushing’s Disease is a hormonal imbalance. Let’s start with how things normally work. The… [...]
What is My Dog’s Life Expectancy With Cushing’s Disease? A Vet Weighs In - Essentially, Cushing’s Disease is a hormonal imbalance. Let’s start with how things normally work. The… [...] When to Euthanize a Dog with Cushing’s disease? [Vet Advice] - Making the decision to euthanize a dog with Cushing’s disease is not an easy one… [...]
When to Euthanize a Dog with Cushing’s disease? [Vet Advice] - Making the decision to euthanize a dog with Cushing’s disease is not an easy one… [...]
Disclaimer: This website's content is not a substitute for veterinary care. Always consult with your veterinarian for healthcare decisions. Read More.




My dog (bichon) was 12 yrs old, had her since she was 4 months old and was having some episodes for about a month, just not feeling herself. I wasn’t really concerned as she was energetic one day and not doing well the the next. She did eat very well, however she did drink a lot of water thought it was from her treat as I know they are a bit salty. Actually, I really did not know she was this sick. She was a fighter, however she was healthy except for one time she had a blood clot in her little bladder. Took her to the vet and on a Sunday night to reveal this. She stayed 2 nights and was fine when I picked her up. I don’t know if anyone is this despondent over a little dog. I should have taken her to the vet when symptoms changed. At the end she did very poorly took her to the vet and unfortunately she was so sick I had to have my Katiegirl put down. I don’t have children or a husband, she was my whole world, just her and I. I’ m searching for another baby but no luck, just a lot of scammers on facebook.I’ m extremely depressed and my health is poor from losing my baby. I hope to get another small dog, hopefully a Bichon, however finances aren’t not good. If you know of any reccomendations please share it with me. And thank you for reading my message.
My heart goes out to you. I just lost my Oscar, Maltese 11 and a half years old with Diabetis and an autoimmune disease that was unknown. After ICU multiple days. Blood tranfusion two weeks later due to Anemia. Broke my heart. I have to say if I ever get another dog, I will first go to an animal shelter. They do have full breed dogs there. I have allergies so I need a smaller dog. If you spent a lot of resources, it might be easier to rescue a fur baby there. I know I spent thousands, (well worth it for my baby). God Bless. Your dog was lucky to have you.