This article was updated on January 16th, 2026
As an emergency veterinarian, there is a very classic presentation I see on a weekly basis. An older, large breed dog will present to my hospital with a sudden history of collapse, weakness, lethargy, or just not doing right at home. I generally can take one look at these dogs and know right away what the underlying diagnosis is. Pale gums, distended abdomen, and a firm mass effect on abdominal palpation and the answer is pretty apparent.
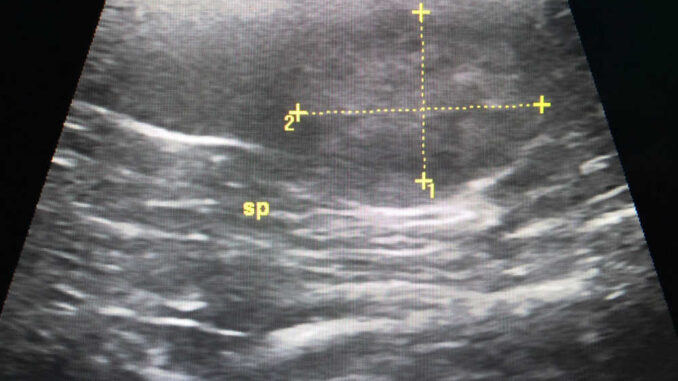
I will use a bedside ultrasound machine to screen the belly, which will generally show free fluid and a mass effect in the upper abdomen. A quick sample of this fluid will demonstrate hemorrhagic (bloody) effusion. My fears have been confirmed. This dog has a hemoabdomen, likely from a bleeding splenic tumor.
Splenic tumors are unfortunately very common in older animals. These tumors may be benign or malignant, but there is no way of knowing without taking the tumor out. This means that owners have to commit to surgery before obtaining an official diagnosis.
Many of these tumors will grow over time but are not diagnosed until the dog shows clinical signs of bleeding. These signs often come on suddenly. Affected dogs may be fine one moment, then the next moment, they are weak and unable to stand. It is a sad diagnosis to have to break to owners, especially because statistically these tumors are caused by an aggressive cancer called hemangiosarcoma.
How Will a Splenic Tumor Affect My Dog?
Splenic tumors are often not diagnosed until they begin bleeding or are diagnosed incidentally. These tumors can grow quickly or slowly depending on the underlying cause. Many dogs will be unaffected when the tumors are small or are not bleeding. Some dogs may be lethargic or have abdominal discomfort secondary to the stretch of the capsule of the spleen as the mass grows in size. If the mass is malignant in origin, dogs may overall feel unwell due to the inflammation caused by cancer. Some dogs will lose weight and have a decreased appetite. Waxing and waning weakness is also an insidious sign.
Here are the most common clinical signs demonstrated by dogs with splenic tumors:
- Abdominal distension
- Abdominal pain
- Generalized weakness
- Poor appetite and potential weight loss
- Pale gums
- Labored breathing
- Collapse
- Vomiting
While some of these clinical signs may be subtle, if a tumor bleeds suddenly, dogs can become extremely weak. Some dogs can have a severe rupture of the mass leading to the point of passing away suddenly from blood loss. This is why it is so important for owners to monitor their dogs diligently, especially if it is known that they have a splenic tumor.
“Many of the patients that present to me with a bleeding splenic tumor did not seem unwell just the day before. This devastating disease can present completely out of the blue.”
How Will the Vet Treat a Splenic Tumor?
After a splenic tumor has been diagnosed, either by abdominal radiographs or ultrasound, your veterinarian will come up with a comprehensive treatment plan. Splenectomy (surgery to remove the spleen) is the number one recommendation. This is performed not only to stop the bleeding but also to remove the mass for an official diagnosis. Before surgery, many dogs may need stabilization, especially if they are actively bleeding. Often we will give dogs intravenous fluids, pain medication, and antiarrhythmics if they are showing abnormalities on their ECG. If they are not able to be stabilized with fluids alone, many dogs will need a blood transfusion to combat anemia caused by the sudden bleed. Medications may be given to help try to slow or prevent further bleeding.
If you elect not to take your dog to surgery, your veterinarian will discuss your options. Dogs that are critically ill may sadly require euthanasia. If your pet is stable or can be stabilized, we will often send them home with medication to slow/prevent bleeding.
Can Dogs Survive a Splenic Tumor Without Treatment?
Without splenectomy, many tumors will continue to bleed, leading to life-threatening anemia. The timeframe of when this will occur is unpredictable and can occur within days to weeks to months.
If your dog has hemangiosarcoma, survival is generally only one to two weeks, with death occurring secondary to severe bleeding. Some dogs may live for months, but this is atypical (Source: Today’s Veterinary Practice).
What is the Life Expectancy With Splenic Tumor Treatment?
The most frustrating thing about splenic tumors is that an underlying diagnosis cannot be made without removing the spleen and submitting it for histopathology. This allows a pathologist to look at the tumor cells and determine if they are malignant or benign in origin.
Dogs who have undergone splenectomy and have been diagnosed with benign tumors are often cured. They can live a normal lifespan after recovery.
Dogs diagnosed with hemangiosarcoma who have undergone splenectomy, but not chemotherapy will live for one to three months. With chemotherapy, dogs can live for six months with 10% of dogs living up to a year (Source: CSU Animal Cancer Care Center).
Does Life Expectancy & Survival Rate Vary by Splenic Tumor Stage?
The stage does influence survival. Visceral hemangiosarcoma is divided into three stages
- Stage I: Tumor smaller than 5cm with no evidence of metastasis. Dogs with Stage I disease have a median survival of 5.5 months.
- Stage II: Tumor >5cm, ruptured tumors with regional metastasis, but no distant metastatic disease. Dogs with Stage II disease have a median survival of 2 months
- Stage III: Tumor >5cm, ruptured and has invaded adjacent structures or has distant metastatic disease. Dogs with Stage III disease have a median survival of less than 1 month. Splenectomy is often not recommended with Stage III disease given the grave prognosis (Source: Clinician’s Brief).
How Can I Make My Dog’s Life Better When My Dog Has a Splenic Tumor?
Many dogs with Stage I disease will not know they have a tumor at all. They may experience intermittent discomfort, so you should discuss a pain control regimen with your veterinarian. Dogs with more advanced disease may have limited time as bleeding can occur at any moment. It is important to ensure they do not experience any trauma that could cause a splenic mass to rupture. Some of them may have a decreased appetite or lose weight, so it is important to offer them their favorite foods or give them an appetite stimulant.
Medications to slow bleeding can be purchased from your veterinarian. We most commonly use Yunnan Bayou or aminocaproic acid. These should be given daily, but it is controversial as to whether they improve survival time or not. Discuss palliative care with your veterinarian to ensure your dog is as comfortable as possible.
FAQs
Are Most Splenic Tumors Cancerous in Dogs?
Unfortunately, yes. Of dogs that have splenic tumors, 2/3 to 3/4 of them will be cancerous with hemangiosarcoma being the most common form of cancer.
How Common are Splenic Tumors for Dogs?
Splenic tumors are very common in older animals whether benign or malignant.
What Breeds are Most Likely to Have Splenic Tumors?
Large breed dogs are at an increased risk. This is especially true for German Shepherds, Golden Retrievers, Labradors, and Poodles. It is important to remember that any dog can develop a splenic tumor.
Source: https://www.acvs.org/small-animal/splenic-masses
Can a Dog Live a Normal Life without a Spleen?
Yes! Dogs do not need their spleens to live normal lives.
Should I Have My Dog’s Spleen Removed?
If you wish to control the source of bleeding and offer your dog the best chance at survival, then the answer is yes. Without performing a splenectomy, the mass may cause life-threatening bleeding at any time. Performing surgery will allow the mass to be removed, the bleeding to be controlled, and an official diagnosis to be made. This will also help guide future treatments if needed.
Disclaimer: This website's content is not a substitute for veterinary care. Always consult with your veterinarian for healthcare decisions. Read More.



My 16.5 year old Black female Labrador has a splenic mass of 2.2 cm, found on an ultrasound scan when undergoing other tests. It is not bleeding/ruptured. It is not pushing the wall of the spleen out. She appears very well currently, eating well and wanting two walks a day.
I have agreed with the vet to have an ultra sound every week to check whether it has increased in size or not.
My question is, without surgery (which she cannot have due to liver function compromised) is there an average life expectancy? I feel like we are living with a ticking time bomb and her spleen could rupture at any moment. I absolutely don’t want her to have a terrible death from a ruptured spleen. We are monitoring her for signs (lethargy, pale gums, change in behaviour and appetite) I would really appreciate your advice as to whether we are doing the right thing by weekly ultra sound scan and also any thoughts on life expectancy. Many thanks Janey
We are in a very similar situation and am wondering if you ever got answers on this. I wondered how your dog is doing or how things progressed for her? Our vet feels the tumors on our older dog have already spread and so we will not do surgery either. I don’t want her to be in pain, yet I can’t fathom putting her down while she’s still walking around and looking at us with happy loving eyes. Thank you very much fo0r getting back to ius if you can.
Our 11year old male Malamute/Samoyed revealed a 5cm mass on his spleen and patchy liver (does this mean it has spread?). End of life leaflet was given to us and surgery wasn’t an option from the vet. He is not in pain eating well and on his walks daily.His condition doesn’t warranty euthanasia as he is not suffering but we are concerned reading about a rupture at any time. Can an ultrasound image determine any bleeding, what stage cancer and the life expectancy.
Hi there Jill and I am sorry to hear about this. A liver can appear ‘patchy’ for many reasons and we cannot assume this is cancer spread. Some spleen nodules are benign (not cancerous) and will not spread.
As you say, if his quality of life is good, we would not consider euthanasia right now.
Sadly, internal masses can rupture and this can cause sudden shock and collapse. Signs can come on quickly and may include panting, pale gums, bloating and lethargy. If this were to happen, we’d need to have the dog seen by the local emergency vet right away.
Dr Linda Simon MVB MRCVS
“The information on this website is not a substitute for in-person veterinary care. Always seek advice from your veterinarian if you have concerns about your pet’s medical condition.”
My six year old Cavapoo had a sonogram yesterday that revealed a tumor (suspected to be Mass Cell) on her spleen. The size is slightly larger than a golf ball. I cannot afford life saving measures, nor would I want to put her through the chemo that would be required. Currently she sleeps a lot and occasionally has a fever which responds to antibiotic shots that my vet gives her. Her biggest activity is walking. Other than that she sleeps a lot. What is your guess on life expectancy and is she in pain?
I’m so sorry to hear about this. Your vet is best placed to discuss prognosis here, as they have seen the tumour and have your dog’s medical history. A splenic mast cell tumour is very rare, but presumably has been analysed by the lab after a biopsy? If this type of tumour has been confirmed, sadly lifespan tends to be just a few months when tumours are high grade and aggressive.
However, prognosis is a lot more favourable with low grade tumours, and some dogs live several years.
If a low grade tumour, surgery is usually advised as it has a very high cure rate. The surgery is generally straightforward, and worth considering for most, if the cancer has not spread.
It would not be expected for her to be in pain with this, no.
“The information on this website is not a substitute for in-person veterinary care. Always seek advice from your veterinarian if you have concerns about your pet’s medical condition.”
Thank you for your article. Our 11.5 year old lab X was diagnosed with a large splenic tumour a couple of weeks ago from an ultrasound. They removed it the same day, it turns out that it was the size of a grapefruit, had a slight split recently (she had a funny turn, so I got her into the vets and we think it was this funny turn when it happened) and the body had dealt with it. The tumour was in fact a stromal sarcoma, and we have been told to make the most of her, and that every week we get is a bonus, as it is such a rare cancer, and the tumour was large, they couldn’t find any signs of metastasis, but who knows!
Thank you for your article. Our 11.5 year old lab X was diagnosed with a large splenic tumour a couple of weeks ago from an ultrasound. They removed it the same day, it turns out that it was the size of a grapefruit, had a slight split recently (she had a funny turn, so I got her into the vets and we think it was this funny turn when it happened) and the body had dealt with it. The tumour was in fact a stromal sarcoma, and we have been told to make the most of her, and that every week we get is a bonus, as it is such a rare cancer, and the tumour was large, they couldn’t find any signs of metastasis, but who knows, as this cancer tends to metastasise to the liver, lungs and bones.