As a veterinarian, I have become very familiar with the many types of health problems facing our furry family members. One type of condition that pet parents often wonder about is autoimmune disease, which occurs when the body’s immune system mistakenly attacks its own cells, tissues, or organs.
These conditions can be complicated to diagnose and treat. This article will provide a brief overview of the types of autoimmune diseases that commonly affect dogs, their symptoms, causes, and treatment options.
What is an autoimmune disease?
The immune system ordinarily defends the body against pathogens like bacteria and viruses. In autoimmune diseases (also known as immune-mediated diseases), this system malfunctions and starts targeting healthy cells. There are several different types of immune-mediated diseases seen in dogs. Genetics and environmental factors can both play roles in the onset of these disorders, and in many cases there is also a trigger – such as a toxin, infection, or cancer.
What are notable symptoms of autoimmune diseases in dogs?
The symptoms of autoimmune diseases in dogs vary widely depending on the type of disorder and the specific organs or tissues targeted by the immune system. However, there are some general signs that may indicate an underlying autoimmune condition:
- Lethargy or fatigue
- Weakness
- Loss of appetite or changes in eating habits
- Unexplained weight loss
- Fever
- Persistent infections or difficulty healing
- Skin lesions
- Lameness, pain, or stiffness
- Gastrointestinal upset, such as vomiting and diarrhea
- Neurological signs such as tremors or seizures
- Pale gums or unexplained bleeding
What are common types of autoimmune diseases in dogs?
Immune-Mediated Hemolytic Anemia (IMHA)
IMHA occurs when a dog’s immune system mistakenly destroys its own red blood cells, leading to anemia (low numbers of red blood cells).
- Symptoms: Symptoms associated with anemia include weakness, lethargy, pale gums, rapid or difficulty breathing, and collapse. These dogs are often jaundiced (yellow-tint to skin and mucus membranes) and may have a fever and enlarged spleen.
- Diagnosis: Diagnostic testing involves a complete blood count (CBC) to check red blood cell levels and appearance. A chemistry panel, urinalysis, Coombs tests, auto-agglutination test, and imaging to look for an underlying trigger such as cancer or infection are also part of the workup.
- Treatment: Immediate and aggressive veterinary care is required, often involving blood transfusions and the use of immunosuppressive medications like corticosteroids.
- Prognosis: The prognosis is variable depending on the severity of the condition, the speed of diagnosis and treatment, and the underlying trigger. Approximately 20-75% of dogs die from this condition. There is also a recurrence rate of 11-15%.
This image on CliniciansBrief.com shows an extreme example of severe jaundice in a dog.
Immune-Mediated Thrombocytopenia (ITP)
Immune-mediated thrombocytopenia involves the immune system targeting platelets, which are essential for blood clotting.
- Symptoms: Dogs with ITP are at risk for spontaneous bleeding. These dogs will bruise easily and develop petechiae (small red spots on the skin or gums) and ecchymoses (larger bruises). They can also have nosebleeds or blood in their urine or feces (may appear dark and tarry) and develop symptoms of anemia, including weakness, pale gums, and difficulty breathing.
- Diagnosis: Diagnosis is generally made via a complete blood count and platelet count, along with specialized tests to rule out other causes and look for an underlying trigger.
- Treatment: Emergency veterinary treatment often involves blood transfusions and immunosuppressive medications such as corticosteroids.
- Prognosis: The prognosis varies, but with prompt and appropriate treatment, many dogs can live a normal life. Approximately 80% of these dogs recover, however, relapses are common.
You can also see an image of petechiae and ecchymoses on a dog’s abdomen on ClinicianBrief.com.
Lupus (SLE and DLE)
Lupus in dogs can be of two types—Systemic Lupus Erythematosus (SLE), which can affect multiple organs, and Discoid Lupus Erythematosus (DLE), which primarily affects the skin.
- Symptoms: DLE generally manifests as facial skin lesions, including ulceration and loss of pigment, particularly around the nose and ears. The nose will also become smooth and lose its typical cobblestone texture. Because SLE can affect almost any part of the body, the signs can vary widely from one dog to another, and may include fever, lethargy, joint pain, skin lesions, kidney disease, neurological signs, and more.
- Diagnosis: DLE is diagnosed with skin biopsies. Diagnosis of SLE is more complex and often involves a combination of blood tests, skin biopsies, and imaging. Approximately 95% of dogs with SLE will test positive on an ANA (anti-nuclear antibodies) test, however, the test is not conclusive if used alone.
- Treatment: Corticosteroids and immunosuppressive medications such as cyclosporine are often prescribed to control symptoms. Skin lesions that become infected will require antibiotic treatment as well. Other potential treatments include topical creams and ointments.
- Prognosis: The prognosis for DLE is good, and after skin lesions are fully resolved, medications can be tapered. However, recurrence and flareups are common. SLE is a progressive and unpredictable disease with a guarded prognosis.
This image on VetSkinAndEar.com shows typical lesions on the nose associated with discoid lupus erythematosus. Note the loss of cobblestone appearance and change in pigment.
Immune-Mediated Polyarthritis
Immune-mediated polyarthritis (also known as rheumatoid arthritis) is a chronic condition affecting the joints, causing inflammation and pain.
- Symptoms: Affected dogs may show stiffness, especially after periods of rest, limping, or reluctance to move. Joints may be swollen and warm to the touch. A fever and loss of appetite are also common signs.
- Diagnosis: Diagnosis is typically made through a combination of clinical symptoms, blood tests, joint taps, and imaging studies like X-rays.
- Treatment: Treatment involves anti-inflammatory medications and immunosuppressive drugs to manage symptoms.
- Prognosis: Prognosis is considered guarded due to frequent relapses, however, if diagnosed early and managed well, a happy and healthy life is possible.
Check out this image of swollen joints on CriticalCareDVM.com.
Autoimmune Skin Diseases (Pemphigus Complex)
The Pemphigus complex refers to a group of autoimmune skin diseases that result in lesions on the skin, primarily around the face, lips, eyes, nose, and ears.
- Symptoms: Dogs will display skin abnormalities such as pustules, crusted skin, blisters (vesicles), and hair loss. These symptoms can be painful and affect the dog’s quality of life.
- Diagnosis: A diagnosis requires skin biopsies.
- Treatment: Steroids and immunosuppressive drugs are usually part of the treatment regimen. Topical ointments may also be prescribed.
- Prognosis: Pemphigus vulgaris is rare but has the worst prognosis – unfortunately, this condition is often fatal. However, most dogs suffering from the other types of pemphigus generally do well with appropriate treatment.
Severe skin lesions associated with pemphigus can be seen on this picture.
Myasthenia Gravis (MG)
Myasthenia Gravis is an autoimmune disorder where the immune system attacks the neurotransmitter receptors in the neuromuscular junction. This means that nerve impulses cannot effectively trigger muscle contractions, leading to muscle weakness and exercise fatigue.
- Symptoms: Affected dogs often display generalized weakness, which may worsen with exercise. Regurgitation due to esophageal problems is also commonly associated with this condition, which can result in difficulty swallowing, aspiration of food, and subsequent pneumonia.
- Diagnosis: The Tensilon test (administration of an IV medication) can provide a rapid but temporary improvement in muscle strength, indicating MG. Diagnosis is confirmed through blood tests measuring acetylcholine receptor antibody levels. X-rays are also recommended to evaluate the esophagus and lungs.
- Treatment: Treatment involves anticholinesterase medications like Pyridostigmine bromide to improve nerve-to-muscle signals, along with supportive care for dogs with esophageal issues or pneumonia. Some dogs also need immunosuppressive medications. In some cases, a surgery to remove an associated thymoma (mass in the chest cavity) may be indicated.
- Prognosis: The prognosis varies. Some dogs might experience a one-time episode and recover fully, while others might have recurring or chronic symptoms. The most immediate life-threatening concern is aspiration pneumonia. With early diagnosis and appropriate management, many dogs with MG can lead a good quality of life.
This video demonstrates muscle weakness in a dog with MG, and response to a Tensilon test:
Lymphocytic Thyroiditis
Lymphocytic Thyroiditis is an autoimmune disease where the immune system attacks the thyroid gland, often leading to hypothyroidism over time.
- Symptoms: Signs of the disease can include lethargy, weight gain, and skin issues like hair loss or recurrent skin infections. Behavior changes such as irritability or aggression may also occur.
- Diagnosis: Diagnosis is usually made through a combination of blood tests that check for thyroid hormone levels and the presence of thyroid autoantibodies.
- Treatment: Treatment involves hormone replacement therapy with synthetic thyroid hormones like levothyroxine.
- Prognosis: The prognosis is excellent with appropriate and life-long medication.
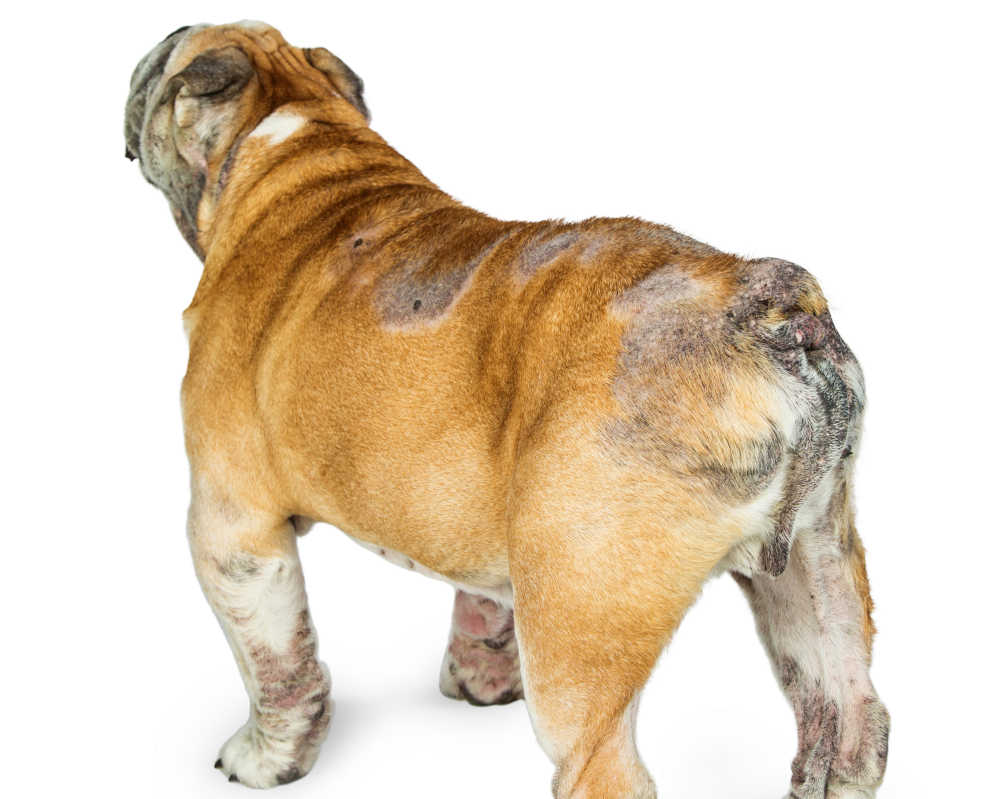
Here is an image of hair loss and scabs as a result of hypothyroidism.
How dogs get autoimmune diseases
The exact cause of autoimmune diseases in dogs is not entirely understood, but it is generally believed to involve several factors, such as genetics and external triggers.
- Genetic predisposition: Certain breeds appear to be more predisposed to specific autoimmune diseases. For example, lupus is more common in German Shepherds and Shetland Sheepdogs, while immune-mediated hemolytic anemia is often seen in Cocker Spaniels. This suggests that genetics may play a role.
- Environmental triggers: Various environmental factors, such as exposure to certain chemicals, toxins, or extreme stress, may trigger an autoimmune response in genetically predisposed animals.
- Infections and cancer: Bacterial or viral infections (especially tick-borne disease) and cancers can initiate autoimmune diseases.
- Drug reactions and vaccines: Certain medications can cause drug-induced autoimmune diseases. For example, certain antibiotics and anticonvulsants have been known to induce autoimmune reactions in susceptible individuals. Vaccines may also play a role in some cases.
What can I do at home to help my dog
There are no home remedies for autoimmune diseases in dogs. These conditions can be severe and life-threatening, and require veterinary testing, treatments, and monitoring.
Is the presence of autoimmune diseases in dogs a reason to be worried? Is it an emergency?
Autoimmune disease in dogs can certainly be a reason for concern. All of these conditions require veterinary care, but the level of urgency depends on the specific condition and symptoms that your dog is experiencing. Some autoimmune conditions can result in severe, life-threatening symptoms that require immediate emergency care. Others may present more gradually and can wait to see your regular vet. Here’s a general breakdown:
Situations Requiring Emergency Attention:
- Immune-Mediated Hemolytic Anemia: If a dog is showing signs of anemia, such as extreme lethargy, rapid breathing, pale gums, or collapse, immediate veterinary attention is necessary, as the condition can be fatal if not promptly treated.
- Immune-Mediated Thrombocytopenia: Signs of spontaneous bleeding and anemia require urgent care.
- Severe Flares of Any Autoimmune Disease: Sudden or extreme symptoms like difficulty breathing, collapse, seizure, bleeding, or severe pain should be treated as emergencies.
Conditions Requiring Prompt but Non-Emergency Attention:
- Lupus (SLE and DLE): While not usually an emergency, symptoms can be severe and have a broad impact on a dog’s health. Timely diagnosis and treatment are crucial.
- Rheumatoid Arthritis: This is generally not an emergency but should be promptly evaluated and treated to improve the dog’s quality of life.
- Lymphocytic Thyroiditis: Although not an emergency, if left untreated, hypothyroidism can result in various health issues.
- Autoimmune Skin Diseases (e.g., Pemphigus Complex): Generally not an emergency but can significantly affect the dog’s quality of life and should be treated in a timely manner.
Regardless of the type or severity, any suspected autoimmune disease in your dog should be addressed by a veterinarian for proper diagnosis and treatment planning. Even “milder” conditions can have a significant impact on your dog’s overall health and quality of life and can lead to more serious complications if not appropriately managed. Therefore, while not every autoimmune disease is an immediate emergency, any sudden or severe symptoms should be treated as such. Always consult your veterinarian for the most accurate advice tailored to your pet’s specific needs.
Your visit at the vet
If you see your vet for concerns about an autoimmune disease, they will always begin by getting a thorough history and performing a nose-to-tail physical exam. Here’s what else you can expect:
Diagnostic Procedures
- Initial consultation ($50-100)
- Bloodwork ($100-300) including CBC and chemistry panel: Used to assess general health, major organ function, and the presence of anemia, infection, or clotting issues.
- Specialized blood tests ($100-300): Such as ANA (Anti-Nuclear Antibody) tests for lupus, Coombs tests for IMHA, and thyroid testing for hypothyroidism.
- Skin Biopsy ($200-800): Common for diagnosing skin autoimmune diseases like pemphigus and lupus.
- Imaging Studies ($100-600): Such as X-rays or ultrasounds to look for abnormalities and conditions affecting internal organs.
- Referral may be needed for advanced imaging and diagnostics in some cases.
Vet Treatments & Costs
- Immunosuppressive Drugs: These are the cornerstone of treatment for most autoimmune disorders. Medications like prednisone and cyclosporine suppress the immune system, thereby reducing its attack on the body’s tissues. Prednisone is generally very affordable, however, other medications may be more costly. It is important to never discontinue these medications without consulting your veterinarian.
- Other medications: Depending on the condition, other medications may include antibiotics to treat infection, pyridostigmine bromide for myasthenia gravis, levothyroxine for hypothyroidism, and other types of medications to manage various symptoms of disease.
- Blood Transfusions: Often required in emergency cases. Dogs who are sick enough to require a blood transfusion will also need to be hospitalized for intensive care and monitoring, which could cost around $5000 or more.
- Supportive Care: Depending on the disease, supportive treatments might include fluid therapy, diet modification, physical therapy, or alternative therapies.
- Regular Monitoring: Autoimmune conditions require extensive follow-up care and medication management. Diagnostic tests such as bloodwork and x-rays will need to be repeated to monitor the progression of disease. This can be a large financial commitment for many pet parents.
Prognosis
It’s essential to understand that while many autoimmune conditions can be managed, they may not always be cured. The prognosis varies widely, depending on factors such as the disease, underlying triggers, your dog’s age and overall health, and their response to treatment. Additionally, the immunosuppressive medications commonly used to treat these conditions can have significant side effects themselves. Unfortunatley, some dogs will die from complications of autoimmune disease, but others can go on to live long and happy lives. Working closely with a veterinarian will ensure the best possible care tailored to your individual dog’s needs.
Disclaimer: This website's content is not a substitute for veterinary care. Always consult with your veterinarian for healthcare decisions. Read More.

